Articles
- Page Path
- HOME > Kosin Med J > Volume 38(1); 2023 > Article
-
Review article
Remote health monitoring services in nursing homes -
Jiwon Kim1,*
 , Hyunsoo Kim1,*
, Hyunsoo Kim1,* , Sungil Im1
, Sungil Im1 , Youngin Park1
, Youngin Park1 , Hae-Young Lee2
, Hae-Young Lee2 , Sookyung Kwon1
, Sookyung Kwon1 , Youngsik Choi1
, Youngsik Choi1 , Linda Sohn3
, Linda Sohn3 , Chulho Oak1
, Chulho Oak1
-
Kosin Medical Journal 2023;38(1):21-27.
DOI: https://doi.org/10.7180/kmj.22.131
Published online: March 29, 2023
1Department of Internal Medicine, Kosin University Gospel Hospital, Kosin University College of Medicine, Busan, Korea
2Department of Chest Surgery, Kosin University Gospel Hospital, Kosin University College of Medicine, Busan, Korea
3Geriatric and Extended Care Service, Department of Veterans Affairs Greater Los Angeles Healthcare System, and Department of Medicine, David Geffen School of Medicine at University of California at Los Angeles, Los Angeles, CA, USA
- Corresponding Author: Chulho Oak, MD, PhD Department of Internal Medicine, Kosin University Gospel Hospital, Kosin University College of Medicine, 262 Gamcheon-ro, Seo-gu, Busan 49267, Korea Tel: +82-51-990-6104 Fax: +82-51-990-3005 E-mail: oaks70@hanmail.net
- *These authors contributed equally to this work as first authors.
Copyright © 2023 Kosin University College of Medicine.
This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 1,263 Views
- 48 Download
Abstract
- Aged people are challenged by serious complications from chronic diseases, such as mood disorder, diabetes, heart disease, and infectious diseases, which are also the most common causes of death in older people. Therefore, elderly care facilities are more important than ever. The most common causes of death in elderly care facilities were reported to be diabetes, cardiovascular disease, and pneumonia. Recently, the coronavirus disease 2019 (COVID-19) pandemic have a great impact on blind spots of safety where aged people were isolated from society. Elderly care facilities were one of the blind spots in the midst of the pandemic, where major casualties were reported from COVID-19 complications because most people had one or two mortality risk factors, such as diabetes or cardiovascular disease. Therefore, medical governance of public health center and hospital, and elderly care facility is becoming important issue of priority. Thus, remote health monitoring service by the Internet of Medical Things (IoMT) sensors is more important than ever. Recently, technological breakthroughs have enabled healthcare professionals to have easy access to patients in medical blind spots through the use of IoT sensors. These sensors can detect medically urgent situations in a timely fashion and make medical decisions for aged people in elderly care facilities. Real-time electrocardiogram and blood sugar monitoring sensors are approved by the medical insurance service. Real-time monitoring services in medical blind spots, such as elderly care facilities, has been suggested. Heart rhythm monitoring could play a role in detecting early cardiovascular disease events and monitoring blood glucose levels in the management of chronic diseases, such as diabetes, in aged people in elderly care facilities. This review presents the potential usefulness of remote monitoring with IoMT sensors in medical blind spots and clinical suggestions for applications.
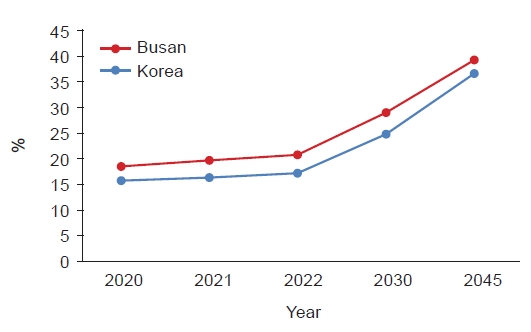
- The entering of a super-aged society and health-related quality of life is becoming more important than ever [1]. The Ministry of Health and Welfare reported a growing super-aged society from 15.7% to 17.3% of the proportion of the population aged 65 and above (Fig. 1). With the rapid entry into a super-aged society, growing socioeconomic problems, which cause sharp increases in chronic disease-related complications, have been reported [1].
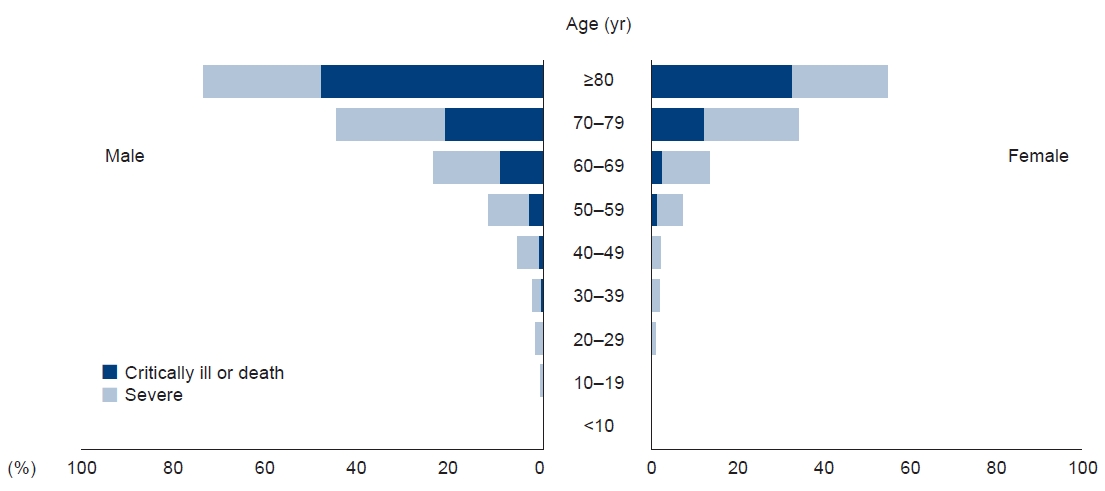
- The number of aged patients with severe illness or death from coronavirus disease 2019 (COVID-19) infections in Korea is significantly high compared to younger patients (Fig. 2) [2]. The recent COVID-19 pandemic caused serious problems in residents in elderly care facilities in Korea, including nursing homes and elderly daycare centers.
- 1. Increasing issue of medical blind spots: elderly care facilities
- The main users of elderly care facilities are aged people with underlying diseases, and the rate of death from COVID-19 infections is very high. Among the total cumulative deaths from COVID-19 in Korea, the number of deaths due to infections in elderly care facilities is high [3,4]. Another outbreak of a COVID-19 strain variant is inevitable, and medical solutions to prepare for infections in elderly care facilities should be considered from a public governance perspective.
- 2. Governance of public health, private health, and care facilities
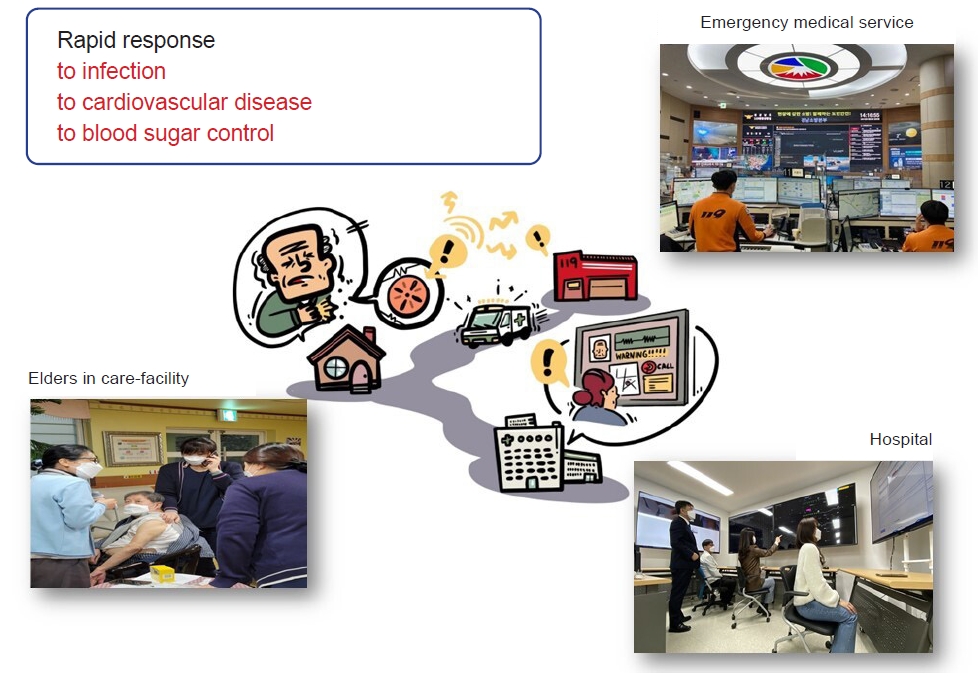
- The main reason for such great casualties in elderly care facilities in the midst of the pandemic was the lack of communication between hospital professionals and medical staff in elderly care facilities. The medical staff of quarantined care facilities were isolated not only spatially but also medically, so no guidance from secondary advisory consultants could be provided [5]. Therefore, the medical governance of public health centers, hospitals, and elderly care facilities is becoming an important issue (Fig. 3).
- 3. Alternative solution for communication between care facilities and general hospitals
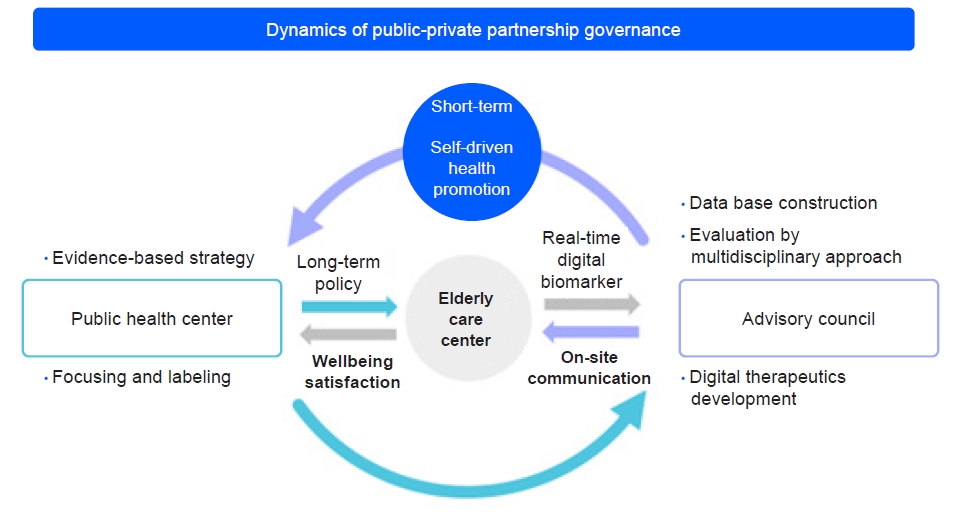
- Based on the above situation, healthcare professionals are greatly challenged to develop new healthcare services to overcome the increasing service burden. The recent development of information, communications, technology technologies has enabled healthcare providers to investigate how to enhance healthcare services in response to the aging population issue [6-8]. Based on smart healthcare and recent innovations, home care technology, such as remote-monitoring services, is becoming a new complementary solution to transform the healthcare industry (Fig. 4).
- 4. Recent breakthrough in remote health monitoring services
- Internet of Medical Things (IoMT)-based remote health monitoring services have been demonstrated as a challenging modality for communicating with elderly care facilities [9,10]. IoMT-based devices, such as real-time electrocardiogram (EKG) monitoring and continuous glucose monitoring sensors, gather digital data using a cloud server [11-14]. The visualization of digital biomarkers from EKG and blood glucose monitoring with a phone gateway helps patients achieve motivation for self-driven lifestyle modifications based on biofeedback from digital data from IoMT sensors (Fig. 5).
Introduction
- 1. Early detection of subclinical cardiovascular and infectious diseases
- Real-time EKG monitoring is clinically useful in the detection of abnormal heart rhythms, such as arrhythmias and coronary diseases [15]. If the real-time EKG monitoring of high-risk patients in care facilities were possible, abnormalities could be detected early and proper medical precautions could be taken. As mentioned above, reports have demonstrated that the real-time EKG monitoring of higher-risk patients with cardiovascular diseases achieved early diagnoses and timely treatment [16]. Therefore, this medical evidence should be extended to applications in care facilities.
- In the field of home care diagnostics, the use of artificial intelligence (AI)-powered diagnostic technologies, such as portable X-ray and ultrasound imaging, for patients in inaccessible areas at home or isolated facilities, is challenging [17-20]. Therefore, AI-powered digital imaging technology connected to real-time EKG monitoring is specifically promising for early detection, and intelligent platforms can assist in decision support and help recognize acute conditions in patients with fatal infectious diseases like COVID-19.
- 2. Evaluation and management of chronic diseases like diabetes
- Well-thought-out blood glucose self-monitoring can monitor a patient's glycemic status [21-23]. IoMT sensors can easily visualize and continuously record blood glucose monitoring data. This can be done mainly by a nurse or medical assistant in care facilities. These data are registered in a cloud server and reviewed by medical professionals, as well as care providers in care facilities, with the consent of the patient (Fig. 6). The patient and caregiver can use the analysis by advisory consultants for timely decision-support messages about the management of chronic diseases, i.e., lifestyle modification or supporting medication [24,25]. This collaboration between care facilities and hospitals may facilitate customized care services to improve the quality of life of patients with chronic diseases.
- 3. Digital literacy of aged people and evaluation of care services
- IoMT-based healthcare services may improve the quality of life for people in care facilities. However, the main obstacle to applying IoMT technology is digital illiteracy. Caregivers must consider the role of medical assistants and nurses in care facilities. Their experiences and motivation for aged people with chronic diseases are essential for achieving remote health monitoring services in care facilities. Therefore, it is vital to establish the digital phenotyping of aged people in regard to simplicity and functionality. Aged people could suffer from a lack of digital experiences, resulting in the impairment of cognitive function [26,27].
Clinically application of IoMT devices in elderly care facilities
- IoMT-based smart healthcare services, especially remote health monitoring services, have become more acceptable. These technologies may provide useful opportunities for preparing safe medical solutions in the midst of the COVID-19 pandemic using real-time patient monitoring resources and services. Real-time EKG monitoring services are used to make early diagnoses of patients with infectious and cardiovascular diseases. Continuous glucose monitoring services have significant potential to achieve the modification of chronic diseases, such as diabetes. Therefore, IoMT sensors may be used to collect useful data from care facilities so that rapid advisory consulting and timely decision-making could be possible for elderly patients.
Conclusion
-
Conflicts of interest
This project was supported by LEENO industrial company. Except for that, no potential conflict of interest relevant to this article was reported.
-
Funding
This work was supported by the Korea Health Industry Development Institute (KHIDI 20210048001).
-
Author contributions
Conceptualization: CO. Data curation: SI. Formal analysis: SK, SI. Funding acquisition: CO. Investigation: HK. Methodology: HYL, YC. Project administration: CO. Software: CO. Supervision: LS. Validation: YC. Visualization: YP. Writing - original draft: JK. Writing - review & editing: CO, JK.
Article information

- 1. Ministry of Health and Welfare. 2020 National Survey of the Living Conditions and Welfare Needs of Older Koreans. Ministry of Health and Welfare; 2021.
- 2. Park HY, Lee JH, Lim NK, Lim DS, Hong SO, Park MJ, et al. Presenting characteristics and clinical outcome of patients with COVID-19 in South Korea: a nationwide retrospective observational study. Lancet Reg Health West Pac 2020;5:100061.ArticlePubMedPMC
- 3. Koff WC, Williams MA. COVID-19 and immunity in aging populations: a new research agenda. N Engl J Med 2020;383:804–5.ArticlePubMed
- 4. Tsang JS, Dobano C, VanDamme P, Moncunill G, Marchant A, Othman RB, et al. Improving vaccine-induced immunity: can baseline predict outcome? Trends Immunol 2020;41:457–65.ArticlePubMedPMC
- 5. Barbera JA, Macintyre AG. Medical surge capacity and capability: a management system for integrating medical and health resources during large-scale emergencies. US Department of Health and Human Services; 2007.
- 6. Klimova B. Mobile health devices for aging population groups: a review study. In: Younas M, Awan I, Kryvinska N, Strauss C, Thanh D, editors. Mobile Web and Intelligent Information Systems. Lecture Notes in Computer Science; 2016. p. 295–301.
- 7. Chung YF, Liu CH. Design of a wireless sensor network platform for tele-homecare. Sensors (Basel) 2013;13:17156–75.ArticlePubMedPMC
- 8. Hollander JE, Carr BG. Virtually perfect? Telemedicine for COVID-19. N Engl J Med 2020;382:1679–81.ArticlePubMed
- 9. Salman OH, Rasid MF, Saripan MI, Subramaniam SK. Multi-sources data fusion framework for remote triage prioritization in telehealth. J Med Syst 2014;38:103.ArticlePubMedPDF
- 10. Mat Kiah ML, Al-Bakri SH, Zaidan AA, Zaidan BB, Hussain M. Design and develop a video conferencing framework for real-time telemedicine applications using secure group-based communication architecture. J Med Syst 2014;38:133.ArticlePubMedPDF
- 11. Damiano ER, McKeon K, El-Khatib FH, Zheng H, Nathan DM, Russell SJ. A comparative effectiveness analysis of three continuous glucose monitors: the Navigator, G4 Platinum, and Enlite. J Diabetes Sci Technol 2014;8:699–708.ArticlePubMedPMCPDF
- 12. Pleus S, Schoemaker M, Morgenstern K, Schmelzeisen-Redeker G, Haug C, Link M, et al. Rate-of-change dependence of the performance of two CGM systems during induced glucose swings. J Diabetes Sci Technol 2015;9:801–7.ArticlePubMedPMCPDF
- 13. Gliner V, Keidar N, Makarov V, Avetisyan AI, Schuster A, Yaniv Y. Automatic classification of healthy and disease conditions from images or digital standard 12-lead electrocardiograms. Sci Rep 2020;10:16331.ArticlePubMedPMCPDF
- 14. De Ridder B, Van Rompaey B, Kampen JK, Haine S, Dilles T. Smartphone apps using photoplethysmography for heart rate monitoring: meta-analysis. JMIR Cardio 2018;2:e4.ArticlePubMedPMC
- 15. Garcia JS, Alonso SG, de la Torre Diez I, Garcia-Zapirain B, Castillo C, Coronado ML, et al. Reviewing mobile apps to control heart rate in literature and virtual stores. J Med Syst 2019;43:80.ArticlePubMedPDF
- 16. Ilbeigipour S, Albadvi A, Akhondzadeh Noughabi E. Real-time heart arrhythmia detection using Apache Spark Structured Streaming. J Healthc Eng 2021;2021:6624829.ArticlePubMedPMCPDF
- 17. Eisenhuber E, Schaefer-Prokop CM, Prosch H, Schima W. Bedside chest radiography. Respir Care 2012;57:427–43.ArticlePubMed
- 18. Mentrup D, Jockel S, Menser B, Neitzel U. Iterative scatter correction for grid-less bedside chest radiography: performance for a chest phantom. Radiat Prot Dosimetry 2016;169:308–12.ArticlePubMed
- 19. Mjolstad OC, Dalen H, Graven T, Kleinau JO, Salvesen O, Haugen BO. Routinely adding ultrasound examinations by pocket-sized ultrasound devices improves inpatient diagnostics in a medical department. Eur J Intern Med 2012;23:185–91.ArticlePubMed
- 20. Mulvagh SL, Bhagra A, Nelson BP, Narula J. Handheld ultrasound devices and the training conundrum: how to get to “seeing is believing”. J Am Soc Echocardiogr 2014;27:310–3.ArticlePubMed
- 21. Polonsky WH, Fisher L, Schikman CH, Hinnen DA, Parkin CG, Jelsovsky Z, et al. Structured self-monitoring of blood glucose significantly reduces A1C levels in poorly controlled, noninsulin-treated type 2 diabetes: results from the Structured Testing Program study. Diabetes Care 2011;34:262–7.ArticlePubMedPMC
- 22. Duran A, Martin P, Runkle I, Perez N, Abad R, Fernandez M, et al. Benefits of self-monitoring blood glucose in the management of new-onset type 2 diabetes mellitus: the St Carlos Study, a prospective randomized clinic-based interventional study with parallel groups. J Diabetes 2010;2:203–11.ArticlePubMed
- 23. Pimazoni-Netto A, Rodbard D, Zanella MT; Diabetes Education and Control Group. Rapid improvement of glycemic control in type 2 diabetes using weekly intensive multifactorial interventions: structured glucose monitoring, patient education, and adjustment of therapy-a randomized controlled trial. Diabetes Technol Ther 2011;13:997–1004.ArticlePubMedPMC
- 24. Lee JW, Kim NK, Park HJ, Lee JY, Choi SY, Lee EM, et al. Obesity and insulin resistance according to age in newly diagnosed type 2 diabetes patients in Korea. Kosin Med J 2016;31:157–66.ArticlePDF
- 25. Kim KH, Kim YH, Seo KW, Yoon KY, Shin YM, Choi YS, et al. Immediate changes of glucose metabolism after gastretomy for early gastric cancer in patients with type 2 diabetes. Kosin Med J 2021;36:25–33.ArticlePDF
- 26. Lion KC, Brown JC, Ebel BE, Klein EJ, Strelitz B, Gutman CK, et al. Effect of telephone vs video interpretation on parent comprehension, communication, and utilization in the pediatric emergency department: a randomized clinical trial. JAMA Pediatr 2015;169:1117–25.ArticlePubMedPMC
- 27. Voils CI, Venne VL, Weidenbacher H, Sperber N, Datta S. Comparison of telephone and televideo modes for delivery of genetic counseling: a randomized trial. J Genet Couns 2018;27:339–48.ArticlePubMedPDF
References
Figure & Data
References
Citations


 KOSIN UNIVERSITY COLLEGE OF MEDICINE
KOSIN UNIVERSITY COLLEGE OF MEDICINE


 PubReader
PubReader ePub Link
ePub Link Cite
Cite