Clinical Manifestations of 6 Cases of Septic Pulmonary Embolism at Increased Risk Recently
Article information
Abstract
Objectives
The aim of this study was to investigate the clinico-radiologic features and microbiologic data of patients with SPE in a tertiary care hospital in Busan.
Methods
We retrospectively analyzed clinical and radiologic features of 6 cases with septic pulmonary embolism that occurred from March 2009 to March 2011 in Dong-A university medical center.
Results
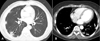
The mean age of the study population was 58 years, and two men and four women were included. Clinical symptoms included general weakness (5 patients), febrile sensation (4 patients) and pleuritic chest pain (2 patients). Underlying conditions were chemoport infection (4 patients), dental abscess (1 patients), and cellulitis of hip (1 patient). Chest computed tomography revealed bilateral multiple nodular opacities in most patients, and cavitation, central necrosis, feeding vessels were identified. All patients received parenteral antimicrobial therapy with or without central catheter removal, drainage of the extrapulmonary infection. Causative organisms were Pseudomonas aeruginosa (2 patients), Candida albicans (1 patient), Bacillus species (1 patient), and Klebsiella pneumonia (1 patient).
Conclusions
Clinical and radiologic features of septic pulmonary embolism were various and nonspecific. The diagnosis was usually suggested by the presence of a predisposing factor of septic pulmonary embolism and CT findings of bilateral multiple nodular opacities in patients with infectious signs and symptoms. Most important underlying condition was intravascular device infection.