Articles
- Page Path
- HOME > Kosin Med J > Volume 37(1); 2022 > Article
-
Original article
Comparison of the radiation dose between dual-acquisition coronary computed tomography angiography and coronary angiography for coronary spasm -
Soo-Jin Kim1
 , Moo Hyun Kim2
, Moo Hyun Kim2 , Eun-Ju Kang3
, Eun-Ju Kang3
-
Kosin Medical Journal 2022;37(1):46-51.
DOI: https://doi.org/10.7180/kmj.21.035
Published online: March 16, 2022
1Division of Cardiology, Department of Internal Medicine, Kosin University College of Medicine, Busan, Korea
2Department of Cardiology, Dong-A University Hospital, Busan, Korea
3Department of Radiology, Dong-A University Hospital, Busan, Korea
- Corresponding author: Moo Hyun Kim, MD Department of Cardiology, Dong-A University Hospital, 26 Daesingongwon-ro, Seo-gu, Busan 49201, Korea Tel: +82-51-240-2976 Fax: +82-51-255-2177 E-mail: kimmh@dau.ac.kr
Copyright © 2022 Kosin University College of Medicine.
This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 2,136 Views
- 31 Download
Abstract
-
Background
- Coronary computed tomography angiography (CCTA) is an imaging technique which can be used to evaluate and diagnose coronary artery stenosis. Dual-acquisition CCTA (DA-CCTA) with additional nitrate infusion is a promising alternative noninvasive diagnostic tool, as conventional CCTA has limitations in the diagnosis of variant angina compared to conventional angiographic coronary spasm tests. However, DA-CCTA may pose a potential risk due to radiation exposure. We compared the radiation dose between DA-CCTA and the coronary angiographic spasm provocation test.
-
Methods
- Patients with clinically suspected variant angina at a single hospital between March 2013 and October 2018 were screened and underwent DA-CCTA or a coronary angiographic spasm provocation test. The effective radiation dose required for each approach was compared.
-
Results
- In total, 211 suspected variant angina patients underwent DA-CCTA or the coronary angiographic spasm provocation test. Of these, 49 patients (mean age, 59.8 years; 67.3% men) received DA-CCTA and 162 patients (mean age, 60.5 years; 66.2% men) received a coronary angiographic spasm provocation test. There was meaningful difference in the effective radiation dose, with a median dose of 5.1 mSv (interquartile range [IQR], 4.1–9.2 mSv) required for DA-CCTA and a median dose of 10.9 mSv (IQR, 8.4–15.2 mSv) for the coronary angiographic spasm provocation test (p<0.001).
-
Conclusion
- DA-CCTA showed a significantly lower effective radiation dose than the coronary angiographic spasm provocation test required to diagnose variant angina.
- The frequency of radiation exposure is increasing in the cardiology field as the application of invasive coronary angiography (CAG) and coronary computed tomography angiography (CCTA) increases [1-5]. In particular, the use of CCTA is increasing as CCTA technology continues to advance [6-8]. For the diagnosis of variant angina, the invasive coronary angiographic spasm provocation test remains the gold standard [9,10]. However, CAG is an invasive procedure requiring catheter insertion into the heart and carries a risk of complications including fetal cardiac arrhythmia. In comparison to CAG, CCTA holds an advantage in being noninvasive, but has limited diagnostic utility in the diagnosis of variant angina [11]. Previous studies have suggested that dual-acquisition CCTA (DA-CCTA) with nitrate infusion may be suitable for the diagnosis of coronary spasm [12,13]. The benefits of DA-CCTA for noninvasive testing include diagnostic feasibility but concerns regarding the risk of two radiological exposures in DA-CCTA remain. In addition, there is little data on the radiation exposure involved in the invasive coronary angiographic spasm provocation test and DA-CCTA in the diagnosis of variant angina [14,15]. Thus, we sought to evaluate the effective radiation dose for DA-CCTA and the invasive coronary angiographic spasm provocation test in the diagnosis of variant angina and determine whether DA-CCTA would be comparable.
Introduction
- Ethical statements: This study was approved by the Institutional Ethics Committee of Dong-A University Hospital (DAUHIRB-17-225). The informed consent was waived because this design is a retrospective study.
- 1. Patient selection
- Patients with clinically-suspected variant angina who visited Dong-A University Hospital in Busan, South Korea, between March 2013 and October 2018 were screened, and all of who underwent DA-CCTA or the invasive coronary angiographic spasm provocation test with available radiation dose information were selected. The final analysis included 211 subjects and we retrospectively collected radiation dose information with clinical data including sex, age, body weight, height, and heart rate.
- 2. Dual-acquisition of CCTA
- DA-CCTA consists of baseline CCTA without vasodilator (CCTA step 1) and nitrate CCTA (CCTA step 2). The CCTA step 1 was performed in the early morning without intravenous nitrate infusion. And the CCTA step 2 was followed by nitrate infusion after the CCTA step 1. Administration of any calcium channel blocker or nitrate substrates was stopped over 3 days before the examination, and beta blockers (carvedilol 12.5 mg) were prescribed to patients presenting with a heart rate over 70 beats per minute. For the CCTA step 2, intravenous nitrate was injected at 2 mg/hr prior to 30 minutes of CCTA for effective vasodilation. All CCTAs were implemented using a 320-detector row scanner (Aquilion ONE, Toshiba Medical Systems, Otawara, Japan) with 320×0.5 mm2 collimation, a 350-millisecond gantry rotation time and 175-millisecond temporal resolution. Tube voltage and current were adjusted using the software (Sure Exposure 3D®, Toshiba Medical Systems). The tube voltage was 120 kVp and the tube current was 130–250 mA. The contrast medium was used as nonionic (iobitridol, Xenetix 350 mgI/mL; Guerbet, Villepinte, France), and 50–60 mL of it was injected intravenously at a rate of 4 mL/s, and then 30 mL of a contrast medium and saline mixture (2:8 dilution) was injected at a rate of 4 ml/s. Automatic bolus trigger system activated computed tomography (CT) scan in the ascending aorta with a delay of 5 seconds. Under sufficiently slow heart rate condition (≤65 beat/min), CT scans were acquired with prospectively triggered data collection at 70%–80% of the RR interval. When the heart rate was relatively rapid (>65 beat/min), CT scans were obtained by retrospective data acquisition with electrocardiography (ECG)-based tube current modulation (full tube current 30%–80%). In the few cases with rapid and irregular heart rates, the images were generated using multisegment reconstructions of the heartbeats according to the default values of the CT scanner. The images were subjected to iterative reconstruction processing reconstruction (AIDR 3D, Toshiba Medical Systems). The images were obtained with a thickness of 0.5 mm and an interval of 0.5 mm, and the axial image was reconstructed according to the heart size of each individual. All images obtained were analyzed using the software (Aquarius iNtuition Edition ver. 4.4.11; TeraRecon Inc., Foster City, CA, USA). Reconstructed images from the 75% cardiac phase or the automatically suggested “best phase (ms)” were used for interpretation. For some cases with rapid heart rates, additional systolic or diastolic phase images were used.
- 3. Coronary angiographic spasm provocation test
- CAG was performed using a Allura Xper FD 10/10 (Philips Medical Systems Nederland B.V, Eindhoven, Netherlands). Coronary angiographic spasm provocation test was consisted of the baseline CAG (CAG step 1) and the ergonovine provocation test (CAG step 2). The CAG step 1 was performed on the left coronary artery and then on the right coronary artery. In the CAG step 2, coronary artery spasms were induced by administration of ergonovine (10–20 μg) in the coronary artery only if there was less than 50% vessel stenosis. When coronary artery spasms were induced after CAG in the right coronary artery, they were controlled by injecting nitroglycerin into the coronary artery. If coronary artery spasms were not observed following right CAG, an induction test for the left coronary artery was performed. The ergonovine was injected (10–20 μg) into the coronary artery. Each of the left and right coronary arteries was dosed up to 3 times at 1-minute intervals.
- The positive determination for the ergonovine provocation test was based on the findings for myocardial ischemia (angina symptom or ischemic ECG changes: transient ST segment elevation, ST segment elevation above 0.1 mV, or transient depression) with total or subtotal occlusion, which temporarily reduced the diameter of the coronary artery by more than 90% (negative U-wave was recorded).
- 4. Radiation dose estimates
- Effective radiation doses are expressed in mSv units, and the effective radiation dose for CCTA was calculated by multiplying the dose-length-product by the European Working Group for Guidelines on Quality Criteria in CT conversion coefficient (k=0.014 [mSv]/[mGy×cm]) [16,17]. For CAG, the effective dose was calculated using a coefficient for converting the dose area product to the effective dose (k=0.18 [mSv]/[Gy×cm2]) [18].
- 5. Statistical analysis
- Data analysis was performed using statistical analysis software (SPSS version 18; SPSS Inc., Armonk, NY, USA). Continuous variables are expressed as mean±standard deviation or median with interquartile range (25th and 75th percentiles); nominal variables are expressed as frequencies and/or percentage, as appropriate. The Kolmogorov-Smirnov test was used to test whether data are normally distributed and the chi-square test was used to evaluate proportions of categorical data. Systematic differences between the two groups were assessed using independent Student t-test or Mann-Whitney U test. Differences of effective radiation dose between the CCTA group and the CAG group presented as median/mean value and p-value estimated by Mann-Whitney U test. In addition, we performed generalized linear model by using age, sex, and body mass index (BMI) and estimated mean (standard error). Differences between the CAG step 1 and the CAG step 2, and differences between CCTA step 1 and CCTA step 2 were evaluated using paired t-test or Wilcoxon rank-sum test. Comparison of the radiation doses according to diagnosis was assessed by using one-way analysis of variance test or Kruskal Wallis test. A p-value <0.05 was considered statistically significant.
Methods
- The baseline clinical characteristics of the patients are shown in Table 1. The mean age was 60.4 years old, and 65.4% were male. There were no significant differences in age, sex, or BMI between the two groups.
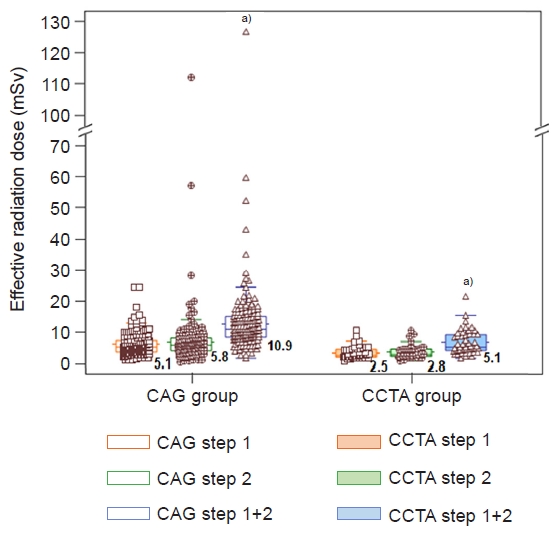
- The effective radiation dose was significantly higher in the CAG group than in the CCTA group (median [IQR]: 10.9 [8.4–15.2] mSv vs. 5.1 [4.1–9.2] mSv, p<0.001) (Fig. 1). Moreover, age, sex, BMI adjusted mean value were significantly higher in the CAG group than the CCTA group (mean±standard error: 7.4±1.5 mSv vs. 13.5±0.9 mSv, p<0.001) (Table 2).
- For the CCTA group, there was no significant difference in the effective radiation dose between the CCTA step 1 and the CCTA step 2 (median [IQR]: 2.5 [2.0–4.5] mSv vs. 2.9 [2.2–4.5] mSv, p=0.162). The radiation dose and heart rate data on the CCTA group is summarized in Table 3. In the CAG group, if the two steps are divided into the CAG step 1 and the CAG step 2, there was a significant difference in the dose area product (median [IQR]: 28.1 [19.6–40.5] Gy·cm2 vs. 32.1 [22.2–44.9] Gy·cm2, p=0.007) and effective radiation dose (median [IQR]: 5.1 [3.5–7.3] mSv vs. 5.8 [4.0–8.1] mSv, p=0.007) between the two steps (Table 3). In the CAG group, the dose area product was different depending on the results of diagnosis (positive, equivocal, negative: 61.1 [47.3–80.3] Gy·cm2 vs. 82.1 [59.0–142.7] Gy·cm2 vs. 54.9 [41.2–86.5] Gy·cm2, p<0.05; post hoc analysis: equivocal>positive=negative) (Fig. 2). In addition, the dose area product noted more significant differences on the CAG step 2 (positive, equivocal, negative: 32.1 [22.5–43.8] Gy·cm2 vs. 53.2 [36.7–85.7] Gy·cm2 vs. 28.0 [15.8–39.7] Gy·cm2, p=0.002; post hoc analysis: equivocal>positive=negative).
Results
- In this study, the CCTA group required a lower effective radiation dose than the CAG group. In addition, the CAG group showed diverse radiation doses according to the results of the provocation test. Conversely, the CCTA group showed no significant differences in the dual acquisition.
- The effective radiation dose for CCTA has been reported as 14.9 mSv and 10.3 mSv in single-source 64 CCTA and dual-source 128 CCTA, respectively [8,14,17,19]. By using a 320-detector row CT scanner, the effective radiation dose can be reduced to a range between 0.58 mSv and 4.0 mSv [19,20]. This study showed a comparable effective radiation dose level for individual CCTA (mean 3.3 mSv) to the recent studies. The radiation dose for CAG has been reported as the dose area product ranging from 23.5 Gy·cm2 to 55.9 Gy·cm2, and coronary angioplasty had a higher level than diagnostic CAG (range, 53.8–101.9 Gy·cm2) [21-23]. In this study, the dose area product for total CAG was 61.4 Gy·cm2, and the constituents (CAG step 1 and CAG step 2) showed a similar radiation dose. However, the results of the spasm provocation test affected fluoroscopic time and radiation dose, and we can expect diverse results according to the requirements of the individual operator. Moreover, there have been few studies of additive radiation doses according to the spasm provocation test in previous reports, and it was found that the radiation dose was over 2-fold higher for diagnostic CAG or was similar to that for coronary angioplasty. In addition, the spasm provocation test via CAG may carry a risk of lethal arrhythmia. Radiation doses have been lowered and quality images can be achieved along with advanced technology, for example, wide-area detector scanners which can make shorter scanning times, helical oversampling, and using an advanced electrocardiogram-gated reconstruction technique. Our findings suggest that the radiation hazard associated with DA-CCTA is less than that for the coronary angiographic spasm provocation test and DA-CCTA may be a good noninvasive diagnostic option for coronary artery disease and coronary artery spasm.
- We acknowledge limitations to this study in that values such as dose length product and dose area product do not allow for comparison between different imaging modalities [14,24]. The radiation dose calculation was performed using a conversion factor from a previous study. However, there are significant variations between previous study results. Additionally, many of the previous studies used 16 detector multi-slice CT [14]. Most of the subjects enrolled in the present study had suitable heart rate and low heart rate variability, although the dose length product of CCTA could be affected by heart rate variability. The patients were not randomized, and the analysis of the data was conducted retrospectively. Furthermore, additional studies such as phantom study for accurate radiation dose comparison was not performed beforehand.
- In conclusion, DA-CCTA showed lower the effective radiation dose than the invasive coronary angiographic spasm provocation test in this study, but with limited clarity.
Discussion
-
Conflicts of interest
This study was partly supported by a research grant from Bayer Co. No other potential conflicts of interest relevant to this article were reported.
-
Acknowledgments
We thank Mr. Won Oh Han (Department of Cardiology, Dong-A University Hospital, Busan, Korea) for his technical assistance and data collections.
-
Funding
This study was partly supported by a research grant from Bayer Co.
-
Author contributions
Conceptualization: MHK. Data curation: SJK. Formal analysis: SJK. Funding acquisition: MHK. Methodology: MHK, EJK. Project administration: MHK. Visualization: SJK. Writing - original draft: SJK. Writing - review & editing: SJK, MHK, EJK. Approval of final manuscript: all authors.
Article information

| Variable | CCTA group (n=49) | CAG group (n=162) | p-value |
|---|---|---|---|
| Effective radiation dose (mSv) | |||
| Median (IQR) | 5.1 (4.1–9.2) | 10.9 (8.4–15.2) | <0.001 |
| Mean±SD | 6.7±3.9 | 13.3±11.7 | <0.001 |
| Mean±SEa) | 7.4±1.5 | 13.5±0.9 | <0.001 |
- 1. Charles M. UNSCEAR report 2000: sources and effects of ionizing radiation. United Nations Scientific Comittee on the Effects of Atomic Radiation. J Radiol Prot 2001;21:83–6.PubMed
- 2. Lucas FL, DeLorenzo MA, Siewers AE, Wennberg DE. Temporal trends in the utilization of diagnostic testing and treatments for cardiovascular disease in the United States, 1993-2001. Circulation 2006;113:374–9.ArticlePubMedPMC
- 3. Chen J, Einstein AJ, Fazel R, Krumholz HM, Wang Y, Ross JS, et al. Cumulative exposure to ionizing radiation from diagnostic and therapeutic cardiac imaging procedures: a population-based analysis. J Am Coll Cardiol 2010;56:702–11.ArticlePubMedPMC
- 4. Harbron RW, Chapple CL, O’Sullivan JJ, Best KE, Berrington de Gonzalez A, Pearce MS. Survival adjusted cancer risks attributable to radiation exposure from cardiac catheterisations in children. Heart 2017;103:341–6.ArticlePubMed
- 5. Harrison D, Ricciardello M, Collins L. Evaluation of radiation dose and risk to the patient from coronary angiography. Aust N Z J Med 1998;28:597–603.ArticlePubMed
- 6. Ghoshhajra BB, Engel LC, Major GP, Goehler A, Techasith T, Verdini D, et al. Evolution of coronary computed tomography radiation dose reduction at a tertiary referral center. Am J Med 2012;125:764–72.ArticlePubMedPMC
- 7. Hohl C, Muhlenbruch G, Wildberger JE, Leidecker C, Suss C, Schmidt T, et al. Estimation of radiation exposure in low-dose multislice computed tomography of the heart and comparison with a calculation program. Eur Radiol 2006;16:1841–6.ArticlePubMed
- 8. Gosling O, Loader R, Venables P, Roobottom C, Rowles N, Bellenger N, et al. A comparison of radiation doses between state-of-the-art multislice CT coronary angiography with iterative reconstruction, multislice CT coronary angiography with standard filtered back-projection and invasive diagnostic coronary angiography. Heart 2010;96:922–6.ArticlePubMed
- 9. Beltrame JF, Crea F, Kaski JC, Ogawa H, Ong P, Sechtem U, et al. International standardization of diagnostic criteria for vasospastic angina. Eur Heart J 2017;38:2565–8.ArticlePubMed
- 10. JCS Joint Working Group. Guidelines for diagnosis and treatment of patients with vasospastic angina (Coronary Spastic Angina) (JCS 2013). Circ J 2014;78:2779–801.ArticlePubMed
- 11. Kang KM, Choi SI, Chun EJ, Kim JA, Youn TJ, Choi DJ. Coronary vasospastic angina: assessment by multidetector CT coronary angiography. Korean J Radiol 2012;13:27–33.ArticlePubMed
- 12. Jin C, Kim MH, Kang EJ, Cho YR, Park TH, Lee KN, et al. Assessing vessel tone during coronary artery spasm by dual-acquisition multidetector computed tomography angiography. Cardiology 2018;139:25–32.ArticlePubMed
- 13. Kang EJ, Kim MH, De Jin C, Seo J, Kim DW, Yoon SK, et al. Noninvasive detection of coronary vasospastic angina using a double-acquisition coronary CT angiography protocol in the presence and absence of an intravenous nitrate: a pilot study. Eur Radiol 2017;27:1136–47.ArticlePubMed
- 14. Coles DR, Smail MA, Negus IS, Wilde P, Oberhoff M, Karsch KR, et al. Comparison of radiation doses from multislice computed tomography coronary angiography and conventional diagnostic angiography. J Am Coll Cardiol 2006;47:1840–5.ArticlePubMed
- 15. Dill T, Deetjen A, Ekinci O, Mollmann S, Conradi G, Kluge A, et al. Radiation dose exposure in multislice computed tomography of the coronaries in comparison with conventional coronary angiography. Int J Cardiol 2008;124:307–11.ArticlePubMed
- 16. Halliburton SS, Abbara S, Chen MY, Gentry R, Mahesh M, Raff GL, et al. SCCT guidelines on radiation dose and dose-optimization strategies in cardiovascular CT. J Cardiovasc Comput Tomogr 2011;5:198–224.ArticlePubMedPMC
- 17. Hausleiter J, Meyer T, Hermann F, Hadamitzky M, Krebs M, Gerber TC, et al. Estimated radiation dose associated with cardiac CT angiography. JAMA 2009;301:500–7.ArticlePubMed
- 18. Betsou S, Efstathopoulos EP, Katritsis D, Faulkner K, Panayiotakis G. Patient radiation doses during cardiac catheterization procedures. Br J Radiol 1998;71:634–9.ArticlePubMed
- 19. Khoramian D, Sistani S. Estimation and comparison of the radiation effective dose during coronary computed tomography angiography examinations on single-source 64-MDCT and dual-source 128-MDCT. J Radiol Prot 2017;37:826–36.ArticlePubMed
- 20. Chen MY, Shanbhag SM, Arai AE. Submillisievert median radiation dose for coronary angiography with a second-generation 320-detector row CT scanner in 107 consecutive patients. Radiology 2013;267:76–85.ArticlePubMedPMC
- 21. Pantos I, Patatoukas G, Katritsis DG, Efstathopoulos E. Patient radiation doses in interventional cardiology procedures. Curr Cardiol Rev 2009;5:1–11.ArticlePubMedPMC
- 22. Stratis AI, Anthopoulos PL, Gavaliatsis IP, Ifantis GP, Salahas AI, Antonellis IP, et al. Patient dose in cardiac radiology. Hellenic J Cardiol 2009;50:17–25.PubMed
- 23. Loomba RS, Rios R, Buelow M, Eagam M, Aggarwal S, Arora RR. Comparison of contrast volume, radiation dose, fluoroscopy time, and procedure time in previously published studies of rotational versus conventional coronary angiography. Am J Cardiol 2015;116:43–9.ArticlePubMed
- 24. Einstein AJ, Moser KW, Thompson RC, Cerqueira MD, Henzlova MJ. Radiation dose to patients from cardiac diagnostic imaging. Circulation 2007;116:1290–305.ArticlePubMed
References
Figure & Data
References
Citations


 KOSIN UNIVERSITY COLLEGE OF MEDICINE
KOSIN UNIVERSITY COLLEGE OF MEDICINE
 PubReader
PubReader ePub Link
ePub Link Cite
Cite


