Articles
- Page Path
- HOME > Kosin Med J > Volume 33(2); 2018 > Article
-
Case Report
A double-knotted pulmonary artery catheter with large loop in the right internal jugular vein: A case report - Kyoung Sub Yoon, Jung A Kim, Jeong In Hong, Jeong Ho Kim, Sang Yoong Park, So Ron Choi
-
Kosin Medical Journal 2018;33(2):240-244.
DOI: https://doi.org/10.7180/kmj.2018.33.2.240
Published online: December 31, 2018
Department of Anesthesiology and Pain Medicine, Dong-A University College of Medicine, Busan, Korea.
- Corresponding Author: So Ron Choi, Department of Anesthesiology and Pain Medicine, Dong-A University College of Medicine, 26, Daesingongwon-ro, Seo-gu, Busan 49201, Korea. Tel: +82-51-240-5390, Fax: +82-51-247-7819, choisr@dau.ac.kr
• Received: August 17, 2017 • Revised: September 18, 2017 • Accepted: October 16, 2017
Copyright © 2018 Kosin University College of Medicine
Articles published in Kosin Medical Journal are open-access, distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 830 Views
- 1 Download
Abstract
- Knotting of a pulmonary artery catheter (PAC) is a rare, but well-known complication of pulmonary artery (PA) catheterization. We report a case of a double-knotted PAC with a large loop in a patient with hepatocellular carcinoma (HCC) undergoing liver transplantation, which has been rarely reported in the literature. A PAC was advanced under pressure wave form guidance. PAC insertion was repeatedly attempted and the PAC was inserted 80 cm deep even though PAC should be normally inserted 45 to 55 cm deep. However, since no wave change was observed, we began deflating and pulling the balloon. At the 30-cm mark, the PAC could no longer be pulled. Fluoroscopy confirmed knotting of the PAC after surgery (The loop-formed PAC was shown in right internal jugular vein); thus, it was removed. For safe PA catheterization, deep insertion or repeated attempts should be avoided when the catheter cannot be easily inserted into the pulmonary artery. If possible, the insertion of PACs can be performed more safely by monitoring the movement of the catheter under fluoroscopy or transesophageal echocardiography.
- A 40-year-old man (weight, 64 kg; height, 174.2 cm) was admitted to our institution for liver transplantation for hepatocellular carcinoma (HCC). This patient had undergone liver resection twice before that led to recurrences. He had no other underlying disease, and his echocardiogram and laboratory results were within normal range.
- Anesthesia was induced via an intravenous injection of 14 mg etomidate and 20 mg cisatracurium, and intubation was performed. For monitoring continuous arterial blood pressure, cannulation was performed on the right radial artery and the dorsalis pedis artery. The femoral vein and the right internal jugular vein (IJV) were cannulated under ultrasound guidance. Particularly, an advanced venous access high-flow device (AVA HF, Edwards Lifesciences LLC, Irvine, California, USA) was used for the cannulation of the right IJV, through which a PAC (Swan-Ganz CCOmbo V, Edwards Lifesciences LLC, Irvine, California, USA) was inserted.
- Although the entry of the PAC into the right ventricle (RV) was confirmed through pressure monitoring via the distal port of the PAC, it could not be inserted into the PA. After 3 attempts with a maximal depth of 50 cm, surgery was started while monitoring CO with FloTracTM. We did not tried any other attempts, including using fluoroscopy or transesophageal echocardiography (TEE) and changing position because of the inexperience of the practitioner. During surgery, we attempted to insert the PAC. After 2 attempts, the PAC was inserted 80 cm deep, incidentally. However, since no wave and electrocardiogram changes were observed, we started deflating and pulled the balloon. At the 30-cm mark, the PAC could no longer be pulled. We decided to examine the PAC with fluoroscopy after surgery and remove it.
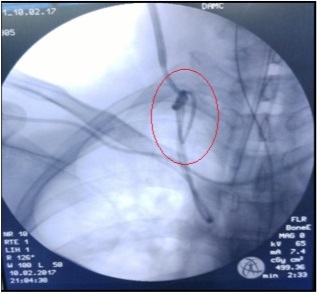
- The fluoroscopic image revealed a double-knotted catheter with a large loop in the right IJV (Fig. 1). A small skin incision was made at the site of PAC insertion, and a venotomy with a purse-string suture was performed on the right IJV by surgeon. Then, the PAC was removed by pulling it through an opening in the center (Fig. 2). The patient was discharged without any complications.
CASE
- The PAC known as the Swan-Ganz catheter, developed by Swan, Ganz, and their colleagues in the 1970s, is used to measure cardiac output, pulmonary capillary wedge pressure, and mixed venous oxygen saturation. It allows for the observation and control of various hemodynamic changes and is still used.1 However, its use has been controversial because it can cause complications such as a balloon rupture, pulmonary infarction, PA rupture, arrhythmias, RV perforation, and knot formation.2 Although there are non-invasive devices for measuring cardiac output, such as lithium dilution cardiac output (LiDCO™), pulse contour cardiac output (PiCCO®), and FloTrac™, their accuracy to measure CO is inferior to that of the PAC with significant aortic regurgitation, arrhythmia, and they have produced different clinical treatment outcomes.3 Therefore, the PAC has been consistently used despite its risks.
- At our institution, a PAC is generally used for monitoring cardiac output and other hemodynamic parameters.
- Knotting of a PAC occurs at a rate of 0.2% to 2.5%, commonly from inserting the PAC 60 cm or deeper without a PA wave or repeatedly performing insertion and withdrawal. Furthermore, a PAC accounts for two-thirds of all intravascular knotted catheters due to its thin and soft wall and long shape.4 To prevent knots, it is important to carefully monitor insertion under pressure wave form guidance. If no PA wave is observed after insertion by an additional 20 cm after observing an RV wave, or if no PA wave appears even after the PAC is inserted 60 cm deep, the balloon must be removed, and the PAC must be gradually pulled back. Changing the patient's position may more effectively prevent PAC knotting.5 With advances in imaging technology, a PAC insertion can be performed aided by other imaging methods. A PAC insertion can be performed under fluoroscopy guidance, which produces real-time animated images using an x-ray, or TEE, which allows for continuous viewing of the cardiac chamber using ultrasound. These methods may enable safer and more accurate positioning of the PAC.56 However, fluoroscopy- or TEE-guided PAC insertion has been not performed at our institution routinely.
- Once a knotted intravascular catheter occurs, various methods can be used to remove it. A PAC can be pulled while a sheath is fixed to reduce the knot size, and then the sheath and PAC can be removed via the insertion site.7 An intervention can be used in which a snaring catheter or wire is used to remove the knot.8 Surgical removal can also be performed.9 Removal of a knotted catheter via an intervention is the safest method because it is less invasive than surgical removal, reduces the knot size, and is less likely to cause vascular trauma; therefore, it has been increasingly used. Herein, the catheter was double knotted with a large loop, and a tail that formed as the tip of the catheter curved, posing a high risk for vascular damage. Because the knot was right beneath the skin, surgical removal was deemed more efficient than an intervention, and was consequently performed. The catheter was removed without any difficulty.
- In summary, to prevent knot formation, a catheter must be sufficiently inserted without balloon inflation, and the use of a catheter with a diameter that is too small should be avoided. Insertion of PACs can be performed more safely by monitoring the movement of the catheter under fluoroscopy or TEE. Deep insertion or repeated attempts should be avoided when the catheter cannot be inserted into the PA. Physicians should be more careful about performing PAC insertions in patients who have RV enlargement, and are more prone to knotting10 or risk factors such as old age, female sex, pulmonary hypertension, coagulation disorders, anticoagulation therapy, and hypothermia.11
DISCUSSION
- 1. Swan HJ, Ganz W, Forrester J, Marcus H, Diamond G, Chonette D. Catheterization of the heart in man with use of a flow-directed balloon-tipped catheter. N Engl J Med 1970;283:447–451.ArticlePubMed
- 2. Lapinsky SE, Richards GA. Pro/con clinical debate: pulmonary artery catheters increase the morbidity and mortality of intensive care unit patients. Crit Care 2003;7:101–103.ArticlePubMed
- 3. Hadian M, Kim HK, Severyn DA, Pinsky MR. Cross-comparison of cardiac output trending accuracy of LiDCO, PiCCO, FloTrac and pulmonary artery catheters. Crit Care 2010;14:R212.ArticlePubMedPMC
- 4. Starzyk L, Yao E, Roche-Nagel G, Wasowicz M. Snaring swans: intraoperative knotting of pulmonary artery catheters. Anaesthesiol Intensive Ther 2016;48:66–70.ArticlePubMed
- 5. Evans DC, Doraiswamy VA, Prosciak MP, Silviera M, Seamon MJ, Rodriquez Funes VR, et al. Complications associcated with pulmonary artery catheters: a comprehensive clinical review. Scand J Surg 2009;98:199–208.ArticlePubMed
- 6. Colbert S, O'Hanlon DM, Quill DS, Keane P. Swan Ganz catheter--all in a knot. Eur J Anaesthesiol 1997;14:518–520.ArticlePubMed
- 7. Böttiger BW, Schmidt H, Böhrer H, Martin E. Non-surgical removal of a knotted Swan-Ganz catheter. Anaesthesist 1991;40:682–686.PubMed
- 8. Karanikas ID, Polychronidis A, Vrachatis A, Arvanitis DP, Simopoulos CE, Lazarides MK. Removal of knotted intravascular devices. Case report and review of the literature. Eur J Vasc Endovasc Surg 2002;23:189–194.ArticlePubMed
- 9. Georghiou GP, Vidne BA, Raanani E. Knotting of a pulmonary artery catheter in the superior vena cava: surgical removal and a word of caution. Heart 2004;90:e28.ArticlePubMedPMC
- 10. Fibuch EE, Tuohy GF. Intracardiac knotting of a flow-directed balloon-tipped catheter. Anesth Analg 1980;59:217–212.ArticlePubMed
- 11. Bossert T, Gummert JF, Bittner HB, Barten M, Walther T, Falk V, et al. Swan-Ganz catheter-induced severe complications in cardiac surgery: right ventricular perforation, knotting, and rupture of a pulmonary artery. J Card Surg 2006;21:292–295.ArticlePubMed
References
Figure & Data
References
Citations
Citations to this article as recorded by 


 KOSIN UNIVERSITY COLLEGE OF MEDICINE
KOSIN UNIVERSITY COLLEGE OF MEDICINE

 PubReader
PubReader ePub Link
ePub Link Cite
Cite


